How technology can save lives when people use drugs alone 2023
While studying epidemiology in graduate school, Ju Park served with a harm reduction organization that taught community people how to prevent drug overdoses. She traversed the state to show how naloxone can reverse opioid overdoses if delivered quickly.
After one session, a mother whose daughter had a substance abuse disorder told Park a heartbreaking story: her daughter had relapsed after several rehab stints. She overdosed in a restroom alone. The mother thanked Park for the naloxone training and said she wanted to help other addiction-stricken families. Park couldn’t tell the mother what she was thinking: Training bystanders to administer naloxone wouldn’t have saved her daughter because nobody was there to help.
“I wondered: What are we doing to help people who use drugs alone and secretly?” Park, an assistant professor of epidemiology and medicine at Brown University’s Warren Alpert Medical School and School of Public Health, remembered.
As she founded Rhode Island Hospital’s Harm Reduction Innovation Lab to develop, implement, and evaluate drug users’ health and well-being, Park kept asking that question.
Overdose detection systems that monitor, detect, and alert responders may be a solution. Park wrote a JAMA Psychiatry column explaining these technologies. The authors are optimistic about these new tools: “Preventing Drug Overdose Deaths.”

Park and her team are doing high-impact research to determine if overdose detection technologies are appropriate for Rhode Islanders and how they can be used to combat the opioid issue nationwide.
Drug usage and dying alone
When Park joined the Brown faculty two years ago, the U.S. Centers for Disease Control and Prevention estimated that roughly half of drug users used alone and 90% of overdoses were unwitnessed. Nearly half of drug users in Baltimore, Providence, and Boston reported using drugs alone, according to a Park-authored study. Park underestimated these amounts.
Solitary drug use is a serious issue: Naloxone can halt overdoses, but a bystander must be trained, equipped, and willing to respond within minutes. As in the mother Park met’s story, when people relapse in secret or take drugs alone, there is no one to help and no time to waste. The data showed that in-the-moment and community-led interventions were needed to supplement overdose prevention initiatives.
Park became interested in overdose detection techniques after meeting the Brave Co-Op at Rhode Island Hospital’s Center of Biomedical Research Excellence (COBRE) on Opioids and Overdose. She conducted the first literature review on overdose detection systems with Boston College, Johns Hopkins, and Brown researchers. The January assessment revealed that few U.S. overdose detection and response technologies are commercially available, though many are in development.
The new JAMA Psychiatry paper by Park, Josiah Rich, and Traci Green, two faculty members from Brown’s public health and medical schools who lead Rhode Island Hospital’s COBRE opioids and overdose research center, examines the feasibility of overdose detection technologies like telephone-based interventions, mobile apps, stationary wired/wireless devices, and wearable biosensors that can monitor movement or oxygen levels. It also suggests a change.
“Amid historical high rates of opioid and nonopioid overdose deaths, social isolation, and other potential health concerns in community settings, novel [overdose detection technologies] are important harm reduction measures to consider evaluating, while existing overdose interventions, such as naloxone and opioid use disorder medications, reach scale,” they wrote.
The methods involve community helpers even if they target drug users alone, the researchers said. The “Never Use Alone” hotline may deploy emergency responders, provide emotional support, and monitor drug usage remotely. Canary and Brave, which require a smartphone, electricity, and internet, allow drug users to anonymously call for help.

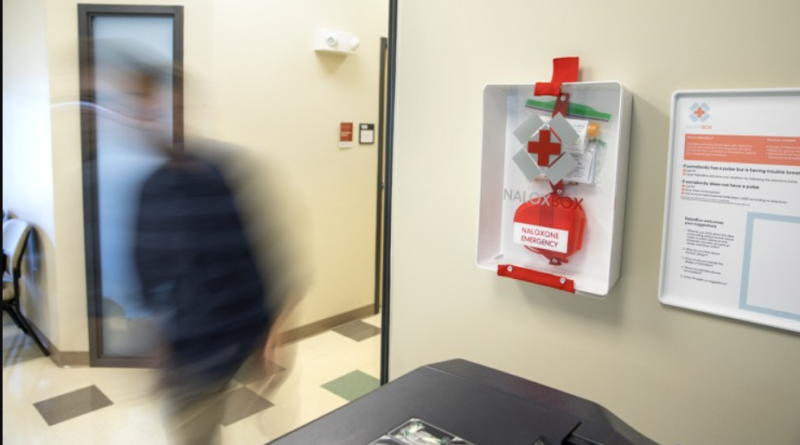
The Brave Button, a wall-mounted wireless gadget, can be used by drug users or onlookers to discreetly send a text alert to pre-trained rescuers, and the Brave Sensor sends an emergency SMS when a person stops moving or breathing. Park said these environmental monitoring may also detect non-drug-related medical situations, such as a person passing out in a library or restaurant bathroom.
Park, Rich, and Green argue for broad overdose detection testing in their paper.
“Technology-assisted interventions will expand overdose prevention if successful,” they conclude.
Community-first technology testing
Park’s lab is researching opioid overdose detection technology as part of the Overdose Detection Technology Project.
The lab is conducting usage training and polling Rhode Island businesses, organizations, and hospitals to see how these initiatives could help Rhode Islanders.
“It’s been eye-opening to learn how many businesses don’t train their staff to use naloxone and have never heard of these technologies, but are interested in learning more,” Park added.
Drug users are being asked in focus groups if and how overdose detection devices fit into their routines.
“We’re trying to understand where the local community is at in applying these technologies, and how we can effectively put them into practice,” Park added.
U.S. and Canadian housing facilities use Brave’s overdose detection systems. Park wants to undertake a randomized trial in Rhode Island to evaluate their efficacy and share the results with other states.
“These life-saving interventions are already in use in different communities, but we don’t know how impactful they can be on a larger scale,” she said.
Park stressed that technology cannot solve overdoses. They may enhance damage reduction efforts.
“The house is burning—100,000 people died from drug overdoses last year, a historical high,” Park remarked. “Crisis mode requires innovative solutions.”